Revised Bethesda Guidelines for testing colorectal tumors for microsatellite instability (MSI)
Tumors from individuals should be tested for MSI in the following situations:
1. Colorectal cancer diagnosed in a patient who is less than 50 years of age.
2. Presence of synchronous, metachronous colorectal, or other HNPCC-associated tumors*, regardless of age.
*Colorectal, endometrial, stomach, ovarian, pancreas, ureter and renal pelvis, biliary tract, brain (usually glioblastoma as seen in Turcot syndrome) tumors, sebaceous gland adenomas & keratoacanthomas in Muir-Torre syndrome, and carcinoma of the small bowel
3. Colorectal cancer with MSI-H histology* diagnosed in a patient who is less than 60 years of age.
*Presence of tumor-infiltrating lymphocytes, Crohn’s-like lymphocytic eaction, mucinous/signet ring differentiation, or medullary growth pattern.
4. Colorectal cancer diagnosed in one or more first-degree relatives with an HNPCC-related tumor, with one of the cancers being diagnosed under age 50 years.
5. Colorectal cancer diagnosed in two or more first-degree relative with HNOCC-related tumors, regardless of age.
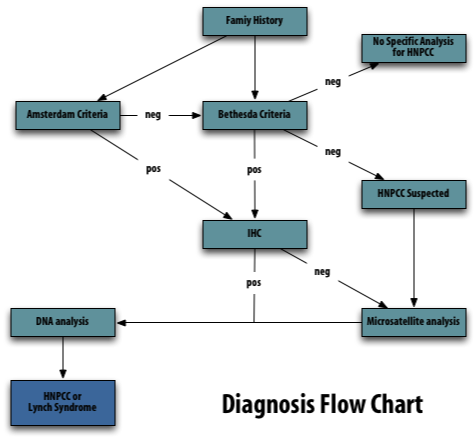
Revised Bethesda Guidelines for Hereditary Nonpolyposis Colorectal Cancer (Lynch Syndrome) and Microsatellite Instability
Download the NIH PDF file HERE.
Download the NIH PDF file HERE.
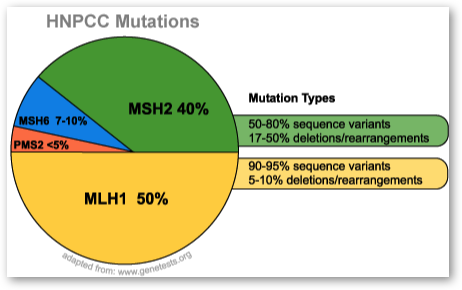
Hereditary non-polyposis colorectal cancer (HNPCC) is usually caused by a mutation in a mismatch repair (MMR) gene. To date, there are four mismatch repair genes linked to HNPCC — MLH1, MSH2, MSH6, and PMS2. Mutations in MLH1 and MSH2 account for about 90% of all HNPCC mutations. Another gene, called EPCAM also interferes with mismatch repair by interaction with the MSH2 gene. It is responsible for a small number of HNPCC cases.